How to Maintain Healthy Feet When Traveling
Traveling is one of life’s greatest experiences — whether you’re exploring a new city, relaxing on vacation, or traveling for business. However, long hours of walking, standing, and sitting can take a toll on your feet and ankles.
A Complete Guide to Preventing Foot Pain and Staying Comfortable on the Go
Many travelers experience foot pain, swelling, blisters, or fatigue during and after trips, often without realizing that simple preventative steps can make a major difference. From long flights to packed itineraries, your feet are constantly under stress while traveling.
The good news is that with the right preparation and habits, maintaining healthy feet for travel is completely achievable. This guide will walk you through essential travel foot care tips to help you stay comfortable, active, and pain-free wherever your journey takes you.
Why Foot Care Is Important While Traveling
Your feet are responsible for absorbing thousands of pounds of Travel puts your feet into situations they may not be used to handling. At home, most people follow relatively predictable routines. They wear familiar shoes, move through familiar spaces, and can rest when needed. Travel disrupts all of that. Suddenly, your feet may be dealing with long stretches of sitting, abrupt increases in walking, hard pavement, unfamiliar shoes, different climates, and a schedule that leaves little time for recovery.
That combination can create a perfect environment for foot pain and inflammation. Long periods of sitting on flights or in cars may reduce circulation and contribute to swelling in the feet and ankles. Then, once you arrive, you may spend hours walking through terminals, hotels, convention centers, tourist attractions, or city streets. If your footwear is not supportive or if your feet are not used to that level of activity, problems can develop quickly.
Foot discomfort during travel is not just about soreness. It can affect the way you walk, change your posture, and place extra stress on your knees, hips, and lower back. A small blister can alter your gait. Swollen feet can make shoes feel tight and uncomfortable. Heel pain can make every step feel more difficult by the end of the day. This is why foot care while traveling is not simply a matter of convenience. It is an important part of protecting your comfort, mobility, and overall health throughout the trip.
For travelers with pre-existing conditions such as plantar fasciitis, bunions, diabetes, arthritis, circulation problems, or chronic ankle instability, thoughtful travel preparation becomes even more important. These individuals are often more vulnerable to irritation, swelling, and pressure-related pain, so a proactive approach can make a meaningful difference.
Common Travel-Related Foot Problems and Why They Happen
Many of the most common foot complaints during travel can be traced back to a handful of causes: poor circulation, prolonged standing, repetitive walking, friction, dehydration, and unsupportive footwear. Understanding what causes these problems is one of the best ways to prevent them.
Swelling in the Feet and Ankles
Swelling is one of the most common complaints among travelers, especially during air travel. When you sit for long periods, blood flow in the lower legs can slow down, and fluid can begin to collect in the feet and ankles. Cabin pressure, inactivity, and dehydration can make this worse. Even after you land, swelling may continue if you are still standing or walking without giving your feet a chance to recover.
Mild swelling is common, but it can still make travel uncomfortable. Shoes may feel tighter, arches may feel more strained, and walking can become more tiring than usual. This is one reason why preventing foot pain on flights often starts with circulation-focused habits.
Blisters and Friction Injuries
Blisters often develop when there is repeated rubbing between the foot, sock, and shoe. New shoes are a common cause, but blisters can also happen when familiar shoes are worn for much longer than usual. Moisture from sweat, rain, or humid environments can make friction worse and soften the skin, which increases the likelihood of irritation.
Travelers who do a lot of sightseeing on foot often realize too late that their shoes are not as comfortable as they thought. A blister on the heel, toe, or ball of the foot can quickly turn a pleasant trip into a painful one.
Heel Pain and Arch Pain
Long days on your feet can aggravate conditions such as plantar fasciitis, especially if your shoes do not provide enough arch support or shock absorption. Hard surfaces like airport floors, sidewalks, cobblestone streets, and concrete walkways can intensify the problem. Even people who do not usually experience heel pain may notice soreness when their activity level suddenly increases.
General Foot Fatigue
Sometimes the issue is not a specific injury but overall exhaustion in the feet and ankles. This often happens when the small muscles in the feet are overworked by long walking days, poor footwear, or inadequate recovery. Your feet may feel achy, stiff, or heavy by the evening, and this fatigue may build over several days if you do not address it.
Skin and Nail Issues
Travel can also create problems such as dry skin, cracked heels, fungal infections, or irritated toenails. Walking barefoot in locker rooms, pools, hotel bathrooms, or spa areas can increase exposure to fungus. Wearing tight shoes for long periods can place pressure on the toenails and surrounding skin, especially if the feet are swollen.
When people think about healthy feet for travel, they often focus only on comfort, but skin integrity and hygiene matter too. A small skin issue can turn into a much bigger source of discomfort if ignored.

Choosing the Right Shoes Before You Travel
One of the most important decisions you can make before a trip is what shoes you are going to bring and what shoes you are going to wear in transit. The right footwear can support your arches, reduce shock, limit friction, and help manage fatigue over long days. The wrong footwear can do the opposite.
A good travel shoe should feel comfortable from the start. It should not need to be “broken in” during the trip. If a shoe is already causing rubbing, tightness, or pressure at home, it is very unlikely to feel better after several hours in an airport or a full day of walking in a new city.
Support matters more than many travelers realize. A supportive shoe helps distribute pressure more evenly across the foot and can reduce strain on the heel, arch, and forefoot. This is especially important for travelers with flat feet, high arches, bunions, or a history of plantar fasciitis. Cushioning is also important because it helps absorb impact, particularly when you are walking on hard surfaces all day.
Breathability is another factor worth considering. Feet tend to swell and sweat more during long travel days, so breathable materials can help reduce moisture buildup and improve comfort. Shoes that are too stiff or too hot can increase both irritation and fatigue.
Travelers often make the mistake of prioritizing appearance over function, especially when packing for a vacation. While style certainly matters, it should not come at the expense of support. If you plan to do significant walking, your primary footwear should be built for comfort, stability, and all-day wear. A good strategy is to pack one reliable, supportive pair as your main shoe and one secondary option for lighter activity or dinner outings.
Why Wearing the Wrong Shoes Can Ruin a Trip

It is difficult to overstate how much footwear affects the travel experience. Many people think they can tolerate a less supportive shoe for a few days, but travel often demands far more from the feet than normal daily life. What feels manageable for a short outing at home can feel completely different after walking five or six miles in a day.
Shoes that are too flat may leave the arches unsupported and increase strain on the plantar fascia. Shoes that are too narrow may compress the toes and worsen bunion pain or cause pressure points. Shoes that are too stiff may rub the heel or limit natural movement. Shoes that are too loose can allow sliding and increase friction, which raises the risk of blisters.
Even a shoe that seems fine at the beginning of the day may become uncomfortable as your feet swell. This is why travelers should think not only about fit at rest, but fit after hours of activity. A shoe that has a little room in the toe box and a secure heel is often a better choice than one that feels snug from the moment you put it on.
For people already dealing with choosing shoes for foot pain at home, travel is not the time to experiment. Bring footwear that has already proven itself under long, demanding conditions.
Preventing Foot Pain on Flights
Air travel presents a unique set of challenges for the feet. Sitting in a confined space for several hours can reduce circulation and contribute to swelling, stiffness, and discomfort. Travelers often stand up at the end of a flight and immediately notice that their shoes feel tighter or their ankles feel puffy. This is one of the main reasons why preventing foot pain on flights requires a specific strategy.
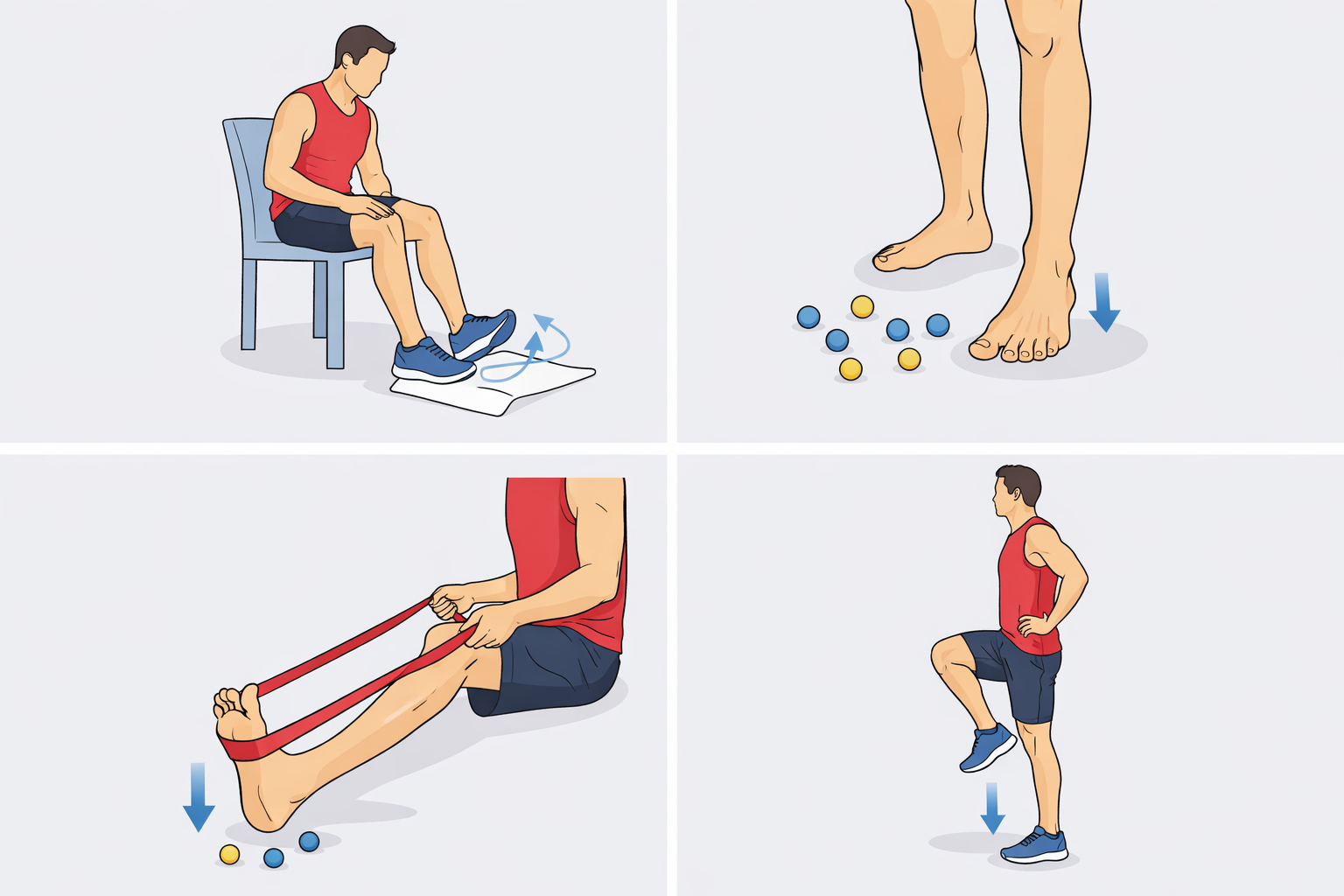
One of the best things you can do during a flight is keep your lower body moving as much as possible. Even if you cannot stand up often, you can still do simple ankle circles, heel raises, toe flexes, and calf contractions in your seat. These small movements encourage circulation and help reduce the sense of stiffness that often builds during long travel.
When it is practical and safe to do so, standing up and walking the aisle can also be helpful. On long-haul flights, taking a brief walk every couple of hours may reduce both swelling and fatigue. Hydration matters too. Dehydration can contribute to sluggish circulation and may make swelling feel worse, so drinking enough water throughout the trip is important.
Compression socks are often a smart option, especially for frequent flyers or travelers prone to swelling. These socks apply gentle pressure to the lower legs and can help promote blood flow back toward the heart. Many travelers find that compression socks reduce heaviness and make it easier to transition from sitting to walking after landing.
It is also wise to avoid excessively tight footwear during a flight. Since the feet often swell in the air, shoes should have some flexibility and room to accommodate that change. Slip-on shoes or supportive sneakers are usually better choices than rigid shoes that already fit tightly on the ground.
How Walking More Than Usual Affects the Feet
A common pattern during travel is moving from a mostly sedentary routine at home to an unusually active one during the trip. A person who normally walks a few thousand steps in a day may suddenly double or triple that number while sightseeing, shopping, or navigating airports. This sudden increase in load can overwhelm tissues that are not used to it.
The feet and ankles are especially vulnerable in this situation because they are responsible for both supporting body weight and helping propel you forward. When activity increases rapidly, the muscles in the arches, calves, and lower legs may become overworked. This can lead to soreness, tightness, and compensation patterns that increase stress on the plantar fascia, Achilles tendon, and joints.
Many travelers notice that their feet feel fine in the morning but progressively worse by the afternoon or evening. That progression is often a sign that the tissues are being overloaded and need more support, more recovery, or both. This is why travel foot care tips should include not only prevention during movement, but recovery after movement as well.
If you know your trip will involve extensive walking, it helps to train for it in advance. That does not necessarily mean a formal exercise program. Even increasing your walking at home in the weeks before a trip can help your feet and lower legs adapt. In addition, packing the right shoes, using supportive insoles if needed, and giving your feet downtime each evening can reduce the likelihood that soreness turns into injury.
Daily Habits That Support Healthy Feet for Travel
The best travel foot care plans are often built on very simple routines. You do not need a complicated system to protect your feet. What matters most is consistency.
At the end of each travel day, it is helpful to check your feet. Look for redness, rubbing, swelling, or developing blisters. Small problem areas are much easier to address early than after they worsen. If you notice a hot spot, applying a protective pad or adjusting your lacing pattern the next day may prevent a blister from forming.
Keeping the feet clean and dry is also important, especially in warm climates or after long walking days. Moisture contributes to friction and can create a more favorable environment for fungal growth. Changing socks when they become damp can make a noticeable difference in comfort. Moisture-wicking socks are often a better choice than standard cotton because they help move sweat away from the skin.
Moisturizing the feet can help maintain skin health, particularly if you are traveling in dry climates or spending time in sandals. Dry, cracked skin is not only uncomfortable, but also more vulnerable to irritation. The exception is the area between the toes, which should generally be kept dry to reduce the risk of fungal issues.
Elevating the feet in the evening can help reduce swelling after long periods of walking or sitting. Even fifteen to twenty minutes with the feet slightly elevated may ease that heavy, tired feeling many travelers experience at the end of the day.
Improper shoes increase risk of ulcers and infection.
How to Prevent Blisters Before They Start
Blisters are one of the easiest travel foot problems to understand and one of the most frustrating to deal with once they develop. Friction, heat, and moisture are the three main ingredients, which means prevention should focus on reducing all three.
The first and most important step is wearing shoes that truly fit. A shoe that rubs slightly at home will usually rub much more after several miles of walking. Socks matter as well. Moisture-wicking socks can reduce dampness and friction, while socks that bunch or slide may make irritation worse.
If there are known trouble spots on your feet, such as the back of the heel or the side of a toe, applying preventive blister pads or friction-reducing products before a long walking day can be helpful. These products work best before damage starts, not after a blister has already formed.
Some travelers also benefit from rotating shoes if possible. Changing footwear from one day to the next can alter pressure patterns and reduce repeated friction in the exact same location. That can be especially useful on longer trips with multiple full walking days.
Blisters may seem minor, but they can change the way you walk and trigger pain in other areas. Preventing them is one of the most practical forms of foot care while traveling.
Special Considerations for Different Types of Travel
Not every trip places the same demands on the feet, so your strategy should reflect the type of travel you are planning.
For air travel, the biggest issues are usually swelling and stiffness from prolonged sitting. Compression socks, hydration, in-seat movement, and flexible footwear are often the most important tools.
For walking-heavy vacations, supportive shoes become the priority. A trip that involves museums, city exploration, tours, or amusement parks often means many hours on hard surfaces. Cushioning, arch support, and pacing become essential. On these trips, it may be wise to build short recovery breaks into the day rather than walking continuously until pain appears.
For beach vacations, different issues arise. Sandals may be convenient, but if they lack support they can aggravate plantar fasciitis or arch strain. In addition, walking barefoot in public shower areas, pool decks, or locker rooms can raise the risk of fungal exposure. Even on a relaxed vacation, healthy feet for travel still require thoughtful choices.
For business travel, the challenge is often balancing professional appearance with comfort. Dress shoes that are worn all day may not provide enough support for repeated walking through airports, conventions, or downtown areas. In these cases, many travelers benefit from packing a more supportive transit shoe and changing into dress shoes only when needed.
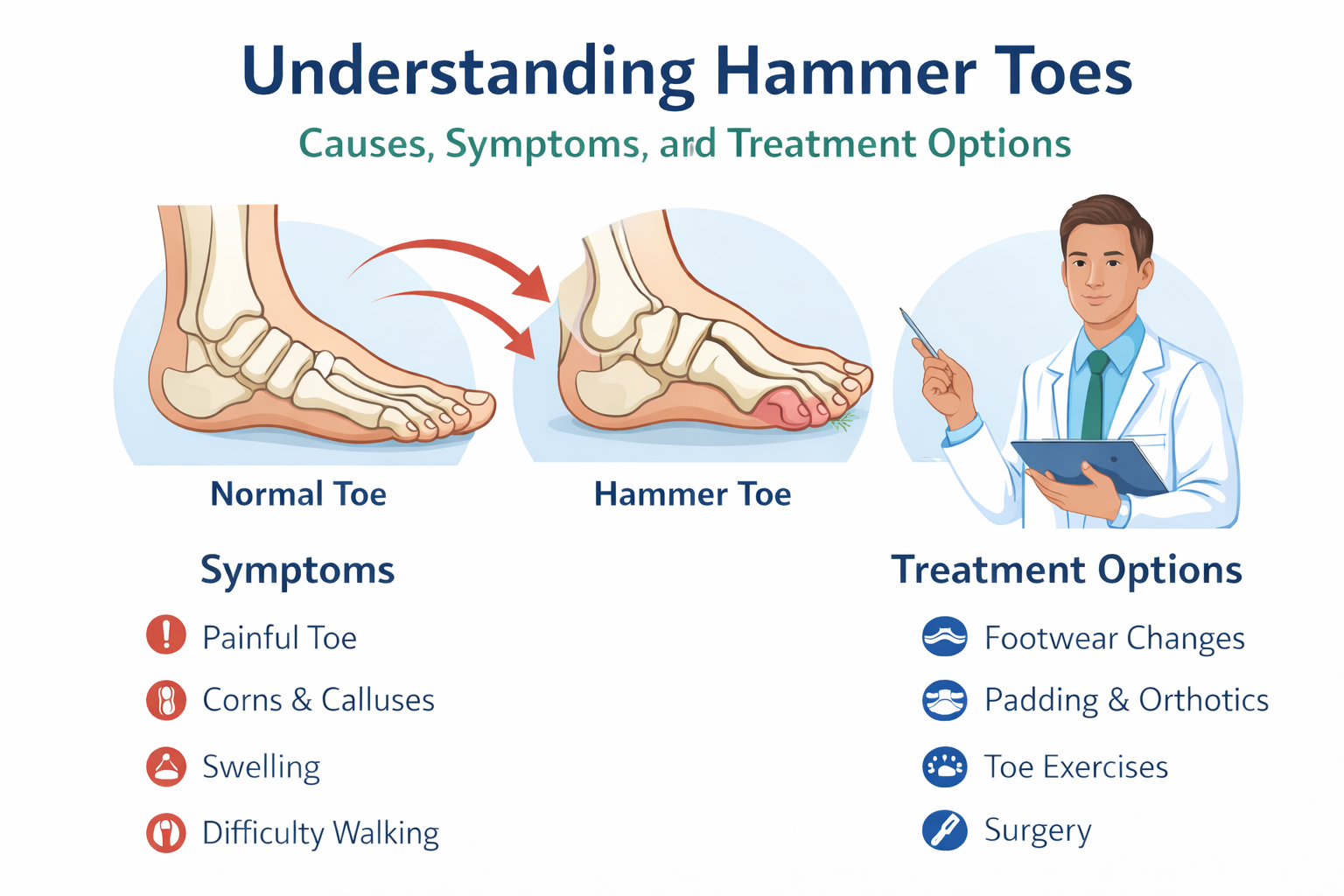
Some travelers need to be especially proactive because they already have foot or ankle problems. Plantar fasciitis, bunions, hammertoes, arthritis, diabetes, tendonitis, and circulation issues can all make travel more difficult if not managed carefully.
For someone with plantar fasciitis, unsupportive sandals or long days on hard pavement can quickly lead to increased heel pain. Supportive shoes with good arch control and cushioning are especially important, and stretching the calves and arches in the morning and evening may help reduce flare-ups.
For those with bunions or forefoot pain, shoe width becomes crucial. Travel shoes should allow the toes enough room to spread naturally without pressure on the joint. Swelling during the day may make a narrow shoe much more painful by evening.
For individuals with diabetes, daily inspection is extremely important. Any rubbing, blistering, or skin breakdown should be taken seriously. Proper foot care while traveling becomes even more essential because small problems may escalate more quickly in diabetic patients, particularly if sensation is reduced.
For people with circulation concerns or swelling issues, compression garments, hydration, and movement during flights or long car rides should be prioritized. These travelers may also want to discuss travel plans with a foot and ankle specialist before a major trip.
What to Pack for Better Travel Foot Care
Packing a few basic items can make it much easier to address issues before they worsen. Travelers often think of foot care as something to deal with only if a problem comes up, but being prepared is usually the better approach.
A supportive pair of walking shoes is the foundation. Beyond that, moisture-wicking socks, compression socks, blister pads, bandages, and a small moisturizer can all be useful additions. Some travelers also benefit from bringing over-the-counter insoles or orthotics if they already use them at home.
If you are prone to heel pain or arch discomfort, packing a massage ball or a small cold pack option may help with end-of-day recovery. While you may not need every item, having even a small foot care kit can make the difference between a manageable issue and a trip-disrupting one.
When Foot Pain During Travel Is a Sign of Something More Serious
Most travel-related foot problems are caused by overuse, swelling, or friction, but not all foot pain should be dismissed as routine. Persistent swelling, severe pain, increasing redness, warmth, numbness, or wounds that do not improve may point to a more serious issue.
For example, if one foot or ankle becomes much more swollen than the other, or if swelling is accompanied by unusual pain, it may warrant medical attention. Likewise, signs of infection such as drainage, spreading redness, or worsening tenderness should not be ignored. Travelers with diabetes should be especially cautious with any skin breakdown or wound.
If foot pain continues after the trip, it may be a sign that the travel demands triggered an underlying condition such as plantar fasciitis, tendonitis, or stress-related irritation. In that situation, professional evaluation can help prevent the issue from becoming chronic.
At Nationwide Foot & Ankle Care, P.C., patients with ongoing foot pain, swelling, irritation, or travel-related flare-ups can receive a thorough evaluation and personalized care plan based on their symptoms and foot structure.
Why Good Travel Foot Care Improves the Entire Travel Experience
When your feet feel good, travel feels easier. You move more comfortably, enjoy activities more fully, and recover better at the end of each day. When your feet are sore, swollen, or blistered, every part of the trip becomes more tiring and less enjoyable. You may cut activities short, walk differently, or lose energy simply because your foundation is hurting.
This is why good travel foot care tips are not small details. They are part of creating a better overall experience. By choosing supportive shoes, managing swelling, protecting your skin, and respecting your body’s limits, you give yourself a much better chance of staying comfortable throughout the trip.
Whether you are planning a weekend getaway, international vacation, cruise, work trip, or long-haul flight, investing in healthy feet for travel is a practical step that pays off quickly. Small preventive choices often make the biggest difference.

The Best Trips Start With Healthy Feet
Selecting the right shoe also depends heavily on how you use it. A shoe that works well for running may not be appropriate for standing all day at work.
Your feet work hard during travel. They support you through airports, city blocks, hotel corridors, beaches, museums, and everything in between. If you want to enjoy your trip fully, they deserve more attention than they usually get.
Maintaining healthy feet for travel starts with preparation and continues with daily habits. Wearing supportive shoes, staying hydrated, moving during flights, managing friction, and checking your feet regularly can all help prevent the most common travel-related problems. These simple steps go a long way toward preventing foot pain on flights and reducing discomfort during long walking days.
If you are already dealing with heel pain, arch strain, swelling, bunions, diabetic foot concerns, or other ongoing issues, it may help to address them before you travel rather than waiting until they interfere with your plans. The right guidance can make travel much more comfortable and less stressful.