How to Protect Your Feet During Long Periods of Standing or Walking:
Spending long hours on your feet is a reality for millions of workers across industries—from healthcare professionals and retail associates to factory workers and hospitality staff. While standing and walking are essential for many jobs, prolonged time on the feet can lead to chronic pain, fatigue, and long-term musculoskeletal issues. Foot health isn’t just about comfort—it’s a cornerstone of mobility, posture, and overall well-being.
Workers who stand for extended periods often experience plantar fasciitis, Achilles tendonitis, stress fractures, bunions, and other painful conditions. Repetitive strain can compromise circulation, weaken muscles, and contribute to joint stress in the knees, hips, and back. Understanding how to protect and strengthen your feet is crucial to maintaining comfort and preventing long-term injury.
At Nationwide Foot & Ankle Care, P.C., our podiatrists in Livonia and Royal Oak, MI, provide comprehensive guidance and treatment for foot pain caused by long hours of standing or walking. From ergonomic footwear and orthotics to stretching, strengthening, and preventive care, we help patients stay active and pain-free.

Understanding Foot Anatomy and Biomechanics
The human foot is a remarkable structure, containing 26 bones, 33 joints, and more than 100 muscles, ligaments, and tendons. It functions as a dynamic support system, absorbing impact, maintaining balance, and propelling the body forward. When standing or walking for long periods, the foot bears the full weight of the body, placing significant stress on its arches, heels, and toes.
Proper foot biomechanics ensures even distribution of pressure across the foot, smooth gait, and minimal strain on muscles and joints. Prolonged standing or walking can disrupt this balance, particularly when combined with hard flooring, poor footwear, or preexisting conditions like flat feet or high arches. Over time, these stresses may cause inflammation, ligament strain, and tendon irritation, potentially leading to chronic conditions such as plantar fasciitis or heel spurs.
Common Foot Problems from Prolonged Standing
SExtended periods on your feet can trigger a variety of foot and ankle problems. Some of the most prevalent issues include:
Plantar Fasciitis: This condition occurs when the thick band of tissue along the bottom of the foot becomes inflamed, often causing stabbing heel pain. Repeated stress from standing or walking can exacerbate plantar fascia strain, particularly in individuals with flat feet or high arches.
Heel Spurs: These bony projections form on the underside of the heel, often in conjunction with plantar fasciitis. They result from repetitive stress and chronic tension on the heel, leading to pain and discomfort during weight-bearing activities.
Achilles Tendonitis: Overuse and tight calf muscles can strain the Achilles tendon, causing inflammation, stiffness, and pain at the back of the heel.
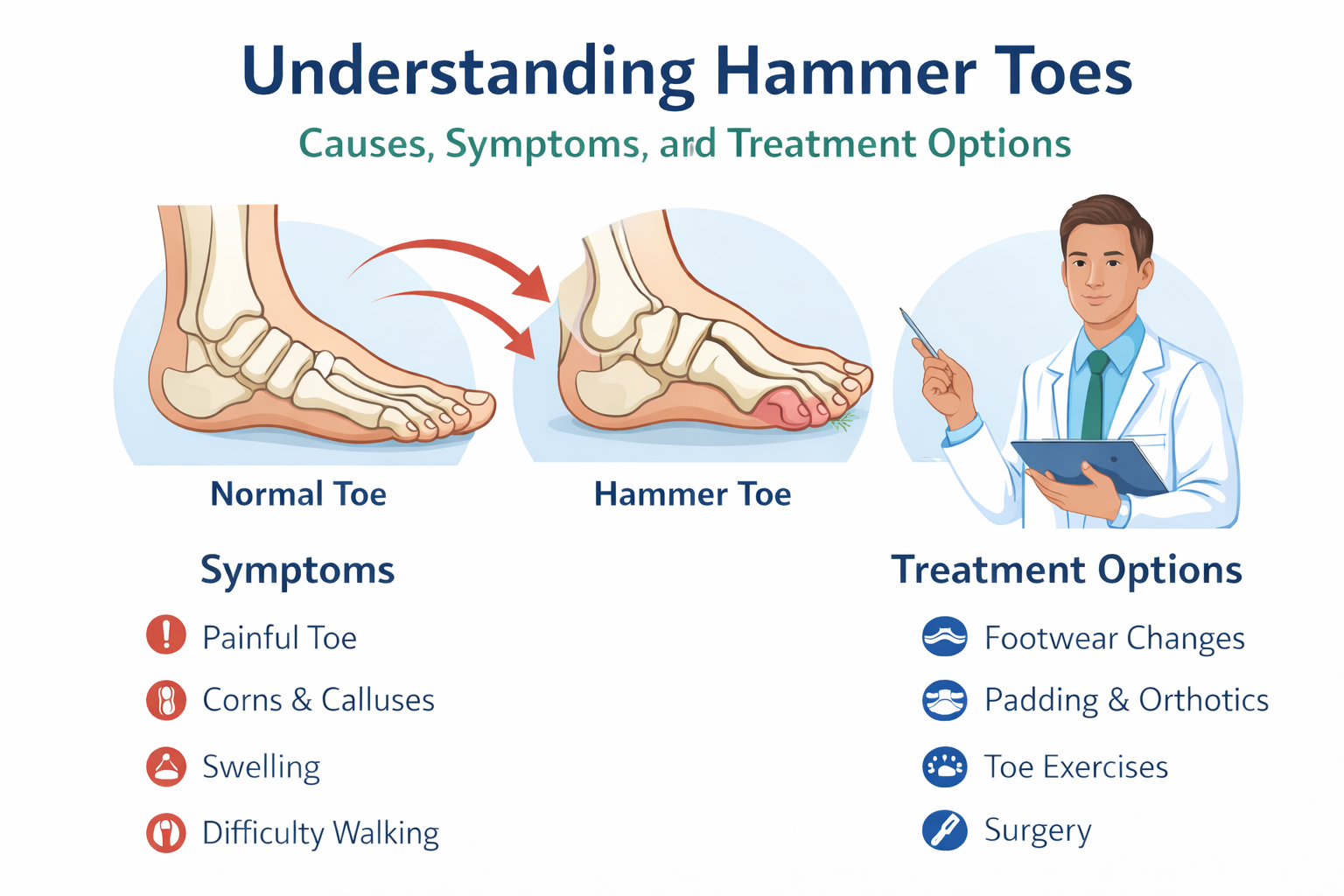
Bunions and Hammertoes: Ill-fitting footwear, genetics, and prolonged pressure can lead to deformities such as bunions and hammertoes, creating pain while walking and limiting footwear choices.
Swelling and Fatigue: Long-standing positions can compromise circulation, causing swelling (edema), heaviness, and a persistent feeling of fatigue in the feet and legs.
Neuropathy and Nerve Irritation: Chronic pressure on nerves in the feet may cause tingling, numbness, or burning sensations, particularly in older adults or patients with diabetes.
By recognizing these risks, individuals can take proactive steps to protect their feet before chronic pain develops.
Early Signs of Foot Stress and When to Seek Help
Mild discomfort can often precede more serious conditions. Warning signs include:
- Persistent heel or arch pain that worsens throughout the day
- Swelling or redness in the feet and ankles
- Tingling or numbness in the toes or soles
- Formation of corns, calluses, or blisters from friction
- Difficulty walking, standing, or maintaining balance
If these symptoms appear, early intervention with a podiatrist can prevent long-term damage, provide guidance on footwear, and initiate treatments like orthotics or physical therapy.
Choosing Supportive Footwear

Footwear is one of the most important factors in protecting your feet during long shifts. Shoes should offer:
- Adequate arch support for your foot type (flat feet vs. high arches)
- Sufficient cushioning in the heel and forefoot
- A wide toe box to prevent pressure points and deformities
- Slip-resistant and breathable materials for safety and comfort
Worn-out shoes, flat-soled footwear, or heels can exacerbate stress on the feet, leading to fatigue, plantar fascia strain, and joint pain. Investing in high-quality, ergonomically designed shoes tailored to your job can reduce discomfort and prevent injuries.
The Role of Custom Orthotics
For many individuals, footwear alone is not enough. Custom orthotics can correct biomechanical imbalances, redistribute pressure, and provide targeted support to relieve pain. They are particularly beneficial for workers with flat feet, overpronation, or high arches.
Orthotics help stabilize the foot, improve gait, and reduce the risk of secondary injuries in the knees, hips, and lower back. Whether prefabricated or custom-made, orthotics can provide relief from plantar fasciitis, heel spurs, bunions, and chronic fatigue associated with standing jobs.
Stretching and Strengthening Exercises for Foot Health
Regular stretching and strengthening exercises are essential for anyone who stands or walks for extended periods. These exercises help maintain flexibility, support arch structures, reduce strain on ligaments, and prevent chronic conditions such as plantar fasciitis, Achilles tendonitis, and heel spurs.
Calf Stretching: Tight calf muscles increase tension on the Achilles tendon and the plantar fascia. Simple calf stretches against a wall or using a step can alleviate pressure and improve mobility.
Plantar Fascia Stretching: Rolling the arch of your foot over a tennis ball or frozen water bottle can help loosen tight fascia and reduce heel pain. Stretching in the morning before standing or walking is particularly beneficial.
Toe and Arch Strengthening: Exercises such as toe curls, picking up small objects with your toes, and towel scrunches help maintain intrinsic foot muscle strength, improve balance, and provide better shock absorption during prolonged standing.
Balance and Proprioception Training: Standing on one leg or using a balance board improves ankle stability, reducing the likelihood of sprains or other injuries.
Ankle Mobility Drills: Gentle rotations, flexion, and extension exercises keep the ankle joints mobile, reducing stiffness and discomfort caused by long-standing positions.
Incorporating these exercises into a daily routine—even 10–15 minutes at the start or end of a shift—can significantly reduce foot fatigue and improve long-term foot health.
Treatment Options for Chronic Foot Pain
Even with preventive measures, some individuals may develop persistent foot pain due to prolonged standing or pre-existing conditions. Early intervention is essential to avoid long-term complications.
Rest and Ice Therapy: Initial management for mild pain or inflammation includes elevating the feet and applying ice to reduce swelling.
Supportive Footwear and Custom Orthotics: Shoes designed for long-standing jobs, coupled with orthotics, help redistribute pressure and provide arch support.
Physical Therapy: Targeted therapy can strengthen foot and ankle muscles, improve flexibility, and correct biomechanical imbalances. Therapists may use modalities such as ultrasound, electrical stimulation, or manual therapy to enhance healing.
Anti-Inflammatory Medications: Over-the-counter NSAIDs can reduce pain and inflammation, while podiatrists may prescribe stronger medications for more severe cases.
Advanced Therapies: Chronic conditions resistant to conservative care may benefit from PRP injections or shockwave therapy to stimulate healing in tendons, fascia, and ligaments.
Surgical Intervention: In rare cases, surgery may be necessary for structural deformities, persistent plantar fasciitis, or severe tendon injuries. Surgery is typically the last resort after a comprehensive trial of conservative measures.
Why Choose Nationwide Foot & Ankle Care, P.C.
OOur podiatrists in Livonia and Royal Oak, MI, are dedicated to providing:
- Expert Diagnosis: Accurate evaluation using advanced imaging and physical assessments.
- Comprehensive Treatment: From conservative care to surgical solutions, tailored to each patient.
- Patient Education: Guidance on preventing recurrence and maintaining long-term foot health.
- Personalized Care: Focused on improving mobility, comfort, and quality of life.
Whether you are an athlete, professional, or someone experiencing daily foot pain, we provide solutions to keep you moving comfortably.
Schedule a Foot and Ankle Consultation
At Nationwide Foot & Ankle Care, P.C., our podiatrists in Livonia and Royal Oak, MI specialize in providing personalized care for workers and individuals with prolonged standing requirements. We focus on prevention, early intervention, and comprehensive treatment options to keep your feet, ankles, and overall posture in optimal condition.
Schedule an appointment today to learn more about customized orthotics, foot strengthening strategies, and other preventative measures for pain-free feet.